31 July 2022: Clinical Research
A Systematic Review of Cross-Sectional Studies Conducted in the Kingdom of Saudi Arabia on Levels of Dental Anxiety Between Genders and Demographic Groups
Mohammed Y. Tarrosh1AEF, Yaser Ali Alhazmi2ABCEG, Mohammed Yahya Aljabri2ACEFG, Mohammed Mousa H. BakriDOI: 10.12659/MSM.937470
Med Sci Monit 2022; 28:e937470
Abstract
BACKGROUND: Dental anxiety can impact oral health and dental treatment in patients of all age groups, which seems to be an obstacle to quality dental care. This systematic review of the literature aimed to evaluate the findings from cross-sectional studies conducted in the Kingdom of Saudi Arabia (KSA) on levels of dental anxiety (DA) between genders and among various demographic groups.
MATERIAL AND METHODS: An electronic search of PubMed, Embase, and Web of Science databases was carried out in January 2022. Studies that measured dental anxiety in Saudis in all regions of the KSA by direct evaluation and interviews were included. Studies that were not in the English language or used proxy measures were excluded. Quality assessment was carried out using Joanna Briggs Institute’s critical appraisal tool for cross-sectional studies.
RESULTS: A total of 19 cross-sectional studies from the KSA were identified that used validated anxiety scales, including the Corah Dental Anxiety Scale (DAS), the Corah Dental Anxiety Scale, Revised (DAS-R), and the Modified Dental Anxiety Scale (MDAS). All studies were rated as having a high risk of bias. A mild level of DA was the most common among participants in the KSA.
CONCLUSIONS: The findings from this systematic review showed that in the KSA, although a mild level of dental anxiety was most common in the study participants, women, young adults, and university students showed a higher prevalence of dental anxiety. However, the lack of sufficient literature to support the current findings make an overall conclusion about DA extremely difficult.
Keywords: Dental Anxiety, Gender role, Prevalence, Saudi Arabia, Cross-Sectional Studies, Female, Humans, Male, Oral Health, young adult
Background
Dental anxiety refers to an emotional state of apprehension or dread at the prospect of dental treatment [1]. The prevalence of dental anxiety (DA) can vary in populations and according to age [2]. It is believed to be 20% or higher based on the population sampled [3–6]. Dental treatment often involves some form of invasive treatment including injections, cavity preparation using high-speed handpieces, or sharp blades and instruments that may be alarming for patients [7]. Subjects suffering from DA report anxiety accompanied by negative thoughts, and fears, coupled with a sense of losing control, linked to a feeling that something dreadful is going to happen in relation to dental treatment [5]. DA may be related to anticipatory anxiety and previous dental experiences of pain and trauma [8].
Dental anxiety can be a significant hindrance to dental care and oral health. Aversion to the dental office and treatment leads to avoidance behavior where the patient does not seek dental care, infrequent attendance, and self-medication in case of pain [9]. Pronounced evasive behavior can lead to missing teeth, decayed teeth, poorer periodontal status, and overall poorer oral health [10–12]. These can undermine growth and development in children and adolescents, predisposing them to systemic disease [13,14]. During treatment, DA can affect compliance and increase the perception of pain, requiring longer treatment times. Delivering resource-intensive care increases the burden of stress on the clinician and staff [15,16].
Studies in population and clinical samples have shown that severe dental anxiety is related to poor mental health [17–19]. Negative consequences in social relationships may include embarrassment regarding poor oral health and decreased self-confidence, as well as increased frequency of absence from work and less social involvement [7,18,20]. Berggren has presented a bio-psychosocial vicious-circle model of dental avoidance, with dentally anxious individuals having poorer dental attendance and more appointment cancellations, leading to poorer oral health [21].
Dental anxiety can vary with age, gender, and ethnicity. DA appears more apparent in females and younger individuals [4,22,23]. Humphris et al, Nascimento et al, Stabholz et al, and Dadalti et al observed that younger and female patients appeared more prone to DA [24–27]. Moore et al dissented from this view, reporting that high dental anxiety was associated with a person’s education, gender, and income but not with age [3]. These variances in the findings may be a result of the methods used to assess the prevalence or the different cultural contexts. Anxiety is inversely related to the frequency of dental attendance, implying that desensitization may be effective [28]. Children with previous caries experience who had not visited dentists may have higher dental anxiety [5].
One other recent cause of DA was COVID-19. Many studies discuss the effect of COVID-19 on dental patients, and there was a significant effect on DA [29–31]. One of the reasons is that the long period of stay at home and the distance between the family members to avoid the infection increase their craving for food, especially sweets, and increase their dental problems [29]. On the other hand, they are anxious about getting infected in the dental office [30]. However, The stress and anxiety increased with the dental practitioner during the COVID-19 pandemic [31]. Nikolić et al found that the COVID-19 pandemic has affected the attitudes and behavior of people about visits to dental offices. Therefore, including a pre-treatment protocol might increase the sense of security for the patient [32,33].
Self-reporting scales allow patient responses to be used to evaluate the level of anxiety. Subjective evaluation by questionnaires, interviews, and self-reporting on anxiety scales can significantly improve the diagnosis and help categorization of these individuals as mildly, moderately, or highly anxious or dental phobics [34]. Various scales and indices have been adopted to record and evaluate DA: Corah’s Dental Anxiety Scale (DAS), Modified Dental Anxiety Scale (MDAS), Corah’s Dental Anxiety Scale-Revised (DAS-R), Dental Fear Survey (DFS), Dental Anxiety Question (DAQ), Depression Anxiety and Stress Scale (DASS); Dental Environment Stress (DES); and Social Anxiety Scale (SAS) [35–43].
Assessment of dental anxiety in a specific population can inform treatment planning and behavior management techniques. A dental team aware of the risk factors for dental anxiety can anticipate a patient’s anxiety and modify their treatment approach [44]. Previously identified factors may vary with population and setting. These findings are crucial for evidence-based dental practice and can inform healthcare decisions. Although dental anxiety is a universal phenomenon, few studies have systematically examined the current literature for evidence of the prevalence of dental anxiety in the Middle East and North African (MENA) countries. Therefore, this systematic review of the literature aimed to evaluate the findings from cross-sectional studies conducted in the Kingdom of Saudi Arabia on levels of anxiety between genders and among demographic groups.
Material and Methods
AIMS OF THE STUDY:
“What is the prevalence of dental anxiety among Saudis in different regions of the Kingdom of Saudi Arabia (KSA)?” We created the focus question with inclusion and exclusion criteria using the PICo framework recommended by the Joanna Brigg Institute for examining qualitative studies [45].
INCLUSION CRITERIA:
The inclusion criteria were: population (P), which included the Saudi population in different regions of the KSA; interest (I), which included experiences in dental anxiety validated using self-examination questionnaires and indices such as Corah’s Dental Anxiety Scale (DAS), Modified Dental Anxiety Scale (MDAS), and Corah’s Dental Anxiety Scale-Revised (DAS-R); and context (Co) of dental care.
EXCLUSION CRITERIA:
The exclusion criteria were: use of proxy measures of dental anxiety, and articles in languages other than English.
SEARCH STRATEGY:
The electronic databases PubMed, Science Direct, Scopus, Wiley Library, and Web of Science were searched for relevant articles. The searches were conducted from July 2021 to August 2021. The search terms used were “dental anxiety,” “scale,” “indices,” and “Saudi Population.” The keywords were used individually or in combination by using the Boolean operators “AND,” “OR,” and “NOT” to search for the term “dental anxiety” independently. The gray literature was searched using Google Scholar.
STUDY SELECTION:
Two reviewers (T.A.A. and M.M.A.) independently assessed articles for eligibility based on the inclusion criteria. After the removal of duplicates, the titles and abstracts of the remaining articles were examined for relevant studies. A third reviewer (P.S.) evaluated the validity and duplications of the studies. Studies that did not assess the level of DA among Saudis, longitudinal studies, case–control studies, systemic reviews, and case reports were excluded. Articles that did not indicate the number of subjects and participants or whose samples had been partly evaluated in other studies were also excluded. A study was deemed relevant when both the researchers agreed that it was related to the study questions.
The full text of potentially relevant articles was obtained and assessed. The references of selected articles were examined for additional studies that fulfilled the inclusion criteria. In case of a disagreement regarding the inclusion of an article, a third reviewer (P.S.) was consulted.
DATA EXTRACTION AND ANALYSIS:
Two authors (T.A.A. and M.M.A.) independently extracted the relevant data from each study using customized tables in Microsoft Excel (Microsoft Corp., Redwood, CA, USA). Any disagreements were resolved through discussion with a third author (P.S.). Details regarding the year of publication, authors, name of city or region, sample size, gender, index or scale used, level of anxiety, outcomes, and significant clinical findings were extracted.
QUALITY OF THE INCLUDED STUDIES:
The quality of the included studies was evaluated using the Joanna Briggs Institute’s critical appraisal tool for cross-sectional studies [45]. The critical appraisal was performed independently by 2 authors (T.A.A. and M.M.A.). Any disagreements were resolved through discussion until consensus was reached with a third author (P.S.). The external validity of the studies was assessed by reporting of 3 criteria: the characteristics of the study groups, the appropriateness of the outcome measures, and the statistical measures used.
Results
STUDY SELECTION:
The search strategy yielded 109 results. From these, 50 articles were excluded as they were duplicates or not related to this review. The remaining articles were screened based on title and abstract. Twenty-one studies were excluded because they were case studies [5], reviews [9], or non-valid samples [7]. The full text of 38 articles was extracted for the assessment using predefined eligibility criteria. Nineteen studies were excluded as they did not use questionnaires or indices. A total of 19 papers that met all the inclusion criteria were included in this review. Figure 1 depicts the flow chart.
QUALITY OF THE EVIDENCE:
The risk of bias assessment revealed that all the 19 included studies suffered from methodological limitations. This led to an overall rating of high risk of bias. A majority of the studies showed attrition bias with a lack of responses. There was limited information on how the response rate was managed. The studies did not use any objective measures to examine dental anxiety. The summary of the risk of bias ratings is presented in Figures 2 and 3.
STUDY CHARACTERISTICS:
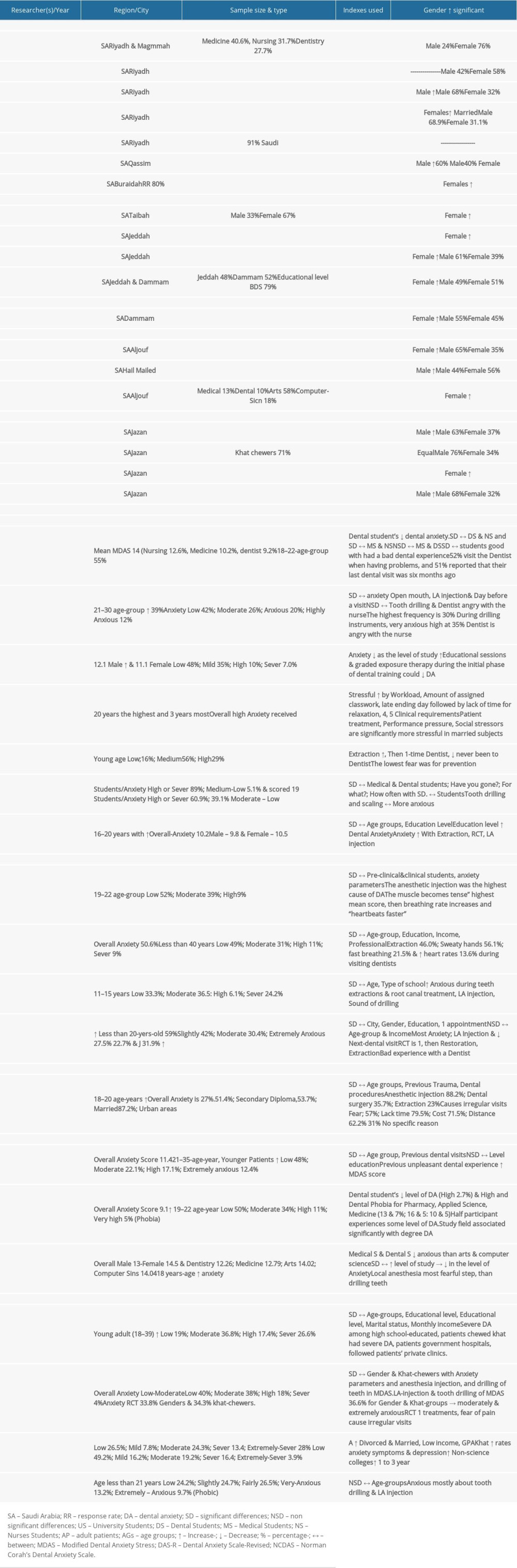
Seven studies were conducted in the central region of the Kingdom of Saudi Arabia (KSA), 4 in the southern and western region, 3 in the northern region, and only 1 in the eastern region. All 7 studies conducted in the central region of the KSA recorded the highest values of all parameters tested, except in “sample size calculation/pilot studies”, where it was only 53%. The score of the parameter “ethics committee”, which most researchers did not include, was 68%. The parameter “future research” was not indicated in 63% of the studies. “Strengths and limitations” was not included in 37% of the studies. “Reliability” and use of intra/interrater reliability tests was not included in 53% of the studies. Only 1 study assessed the level of DA in the eastern region, as compared to 3 and 4 studies that investigated this in the northern and southern regions of the KSA, respectively. Table 1 summarizes the characteristics of the selected studies.
GENDER:
The percentage of male participants (60%) involved in studies on DA in the KSA was higher than that of female participants (40%). Figure 4 shows the studies that reported the incidence of DA among male and female participants in all regions of the KSA. In the western region, 4 studies reported that females had a high DA level [46–49]. In the northern and eastern regions, only 2 studies assessed DA among females and only 1 study evaluated DA among males [50–52]. In the central and southern regions, 3 and 2 studies, respectively, reported high DA levels among males [53–57]. In all regions of the KSA, 10 out of 19 studies reported high DA levels among females.
AGE:
The incidence of DA among young patients (18–39 years old) in all regions of the KSA was reported by 85.5% of the studies. By comparison, 10.5% of the studies reported the incidence of DA among adults (40–59 years old). No study reported the incidence of DA among the elderly (Figure 5) [46,50–53,57–64]. The studies included herein also established that the educational level of the participants was another factor related to DA. Ten studies reported that university students had the highest DA level in all regions of the KSA (Figure 6) [46,50,52,54,58,62–64].
RESPONSE RATE:
The total response rate from all regions was 87.47%. The highest response rate was from the southern region (97%), followed by that from the eastern (93%), western (87.70%), and northern and central regions (80%).
REGIONAL VARIATIONS:
All 5 regions of the KSA had different DA levels (mild, moderate, and severe). The incidence of moderate DA was 40.7% in the western region and 33.6% in the southern region, while the northern region reported the highest incidence of mild DA (79.0%). This, in contrast, was only 31.6% in the central and eastern regions, slightly higher than that of severe DA (29.9%). The incidence of mild (39.7%), moderate (31.1%), and severe (23.4%) DS was substantially different among regions of the KSA (Figure 7).
The other contributing factors did not have a generalized effect on DA in the KSA. Nevertheless, some individual studies that assessed clinical procedures, such as anesthetic injections, surgical procedures, extractions, and tooth drilling, reported that these procedures were terrifying to the patients. Subjects reported that lack of time, unsatisfactory dental services, and fear were attributed to irregular dental visits [46,61]. Two studies also reported that other factors, such as unequal distribution of dental services and the cost of treatment, were contributing factors [46,50].
Discussion
Dental anxiety (DA) is an obstacle to the provision of quality dental care and places an enormous economic, social, and health burden on patients [65]. From a public health standpoint, it is crucial to assess the prevalence DA in a population and examine the factors that may lead to the avoidance of oral healthcare. This systematic review examined the evidence in the literature for the prevalence of dental anxiety in the Kingdom of Saudi Arabia (KSA). The overall DA score in the regions of the KSA was similar, with mild DA being widely reported (39.72%). Reports of DA were high in the northern region (79%). These values were consistent with those reported by Madfa et al [66] among university students in Yemen and those reported by Suhani et al [67] in young participants with hearing impairment in Romania. DA is prevalent regardless of age, gender, social status, and place of residence. This is a growing concern for dental professionals, who need to be aware of the extent of this issue to find systems and procedures that will help patients in overcoming it [49].
The gender distribution of males to females was similar (60% and 40%, respectively). However, the incidence of DA was higher among females. Similar findings were obtained in India, Romania, Yemen, Australia, and Portugal [27,66–69]. There was a disparity in the reports of DA related to gender in the studies included in this review. While 10 studies conducted in the western region of the KSA reported a higher DF level in females, other studies in the central and southern regions of the KSA reported that males had a higher DA level than females, but 2 studies reported that DA level is equal between genders. Earlier reports by Goh et al, Shim et al, and Talo et al concur that females tend to show a greater prevalence of dental anxiety [22,23,44]. However, this is in contrast to other studies that report no variation in dental anxiety between the genders [70], or greater dental anxiety in males [71]. This disagreement among studies may be a result of the cultural background or population examined [72].
We found that the DA level was greater in the younger age group (18–39 years old) as compared to the older age group. Similar findings were reported by studies conducted in Yemen, Romania, and Australia. University students had the highest DA level among all educational groups. Children may be particularly susceptible to influence through second-hand information gleaned from media or reported experiences of family and friends that raise the specter of dental treatment as something “uncomfortable” or “painful” [73]. Past dental experiences may play an outsized role in the development of DA. Feelings of helplessness, duress, and indifference on the part of the dentist may be predictive of future instances of dental anxiety [74]. However, the elderly had the lowest DA level in these studies. This result may be due to sampling bias, as most studies assessed DA levels among college and university students and very few old people participated in these studies.
University students had the highest DA level among all educational groups (10 out of 19 studies). This observation was consistent with that of Caltabiano and Madfa et al in Yemen and Australia. However, it was slightly lower than that reported by Suhani et al, possibly because they only included younger university students [67,69].
The response rate from all the regions of the KSA was very high. This high response rate was achieved because the submission of the questionnaire was followed up during the same visit and most of these studies were conducted in person at location (private clinic, dental centers, or teaching hospital). Females and young adults had a higher level of DA, especially related to clinical procedures. The lack of proper dental health education might have resulted in higher DA levels among nonmedical undergraduates in the country. DA is prevalent regardless of age, gender, social status, or residence. Educational sessions with dental training can help in reducing DA levels among dental students. DA can be reduced through educational campaigns and dental health education. Social media, academic programs, and school- and community-based dental health programs can help educate the populace to reduce the level of DA.
Regarding the completeness and applicability of this research, our review examined studies that used self-reporting via questionnaires to estimate the prevalence of dental anxiety. Self-reporting may be insufficient in delineating levels of dental anxiety. There is considerable variability in the ratings of different scales. Dental anxiety scores need to have a mid-value threshold to be clinically relevant. However, this does not imply that the patients below the clinical threshold have zero anxiety and are relaxed. Stoic and non-demonstrative presentations of anxiety may be difficult to assess in a clinic. It is important to realize that patients who score below the clinical threshold may also need DA management.
There may be a poor agreement between a patient’s anxiety rating and the dentist’s perception. Future studies may benefit from using objective measures such as heart rate, blood pressure, or skin temperature to assess anxiety. Physiological responses such as respiration rate may prove a reliable indicator of dental anxiety level.
There are concerns regarding whether the samples selected can be broadly representative of the general population across all ages. Population-based studies that collect patient-reported outcomes of previous dental experience or caries experience can help in analyzing reasons for ingrained dental anxiety.
The prevalence of dental anxiety is important from both research and clinical standpoints. The findings of this review can help academics focus research on targeted age groups and populations to shift behavior toward a positive attitude to dental care and away from avoidance. Dentistry has evolved technologically through the years, shifting to a digital workflow and newer equipment that may increase patient comfort and reduce dental anxiety [75]. Clinicians aware of an anxious, fearful patient can prepare to meet the emotional needs of the patient. The findings of this review can assist clinicians in identifying, assessing, and treating patients with dental anxiety using pharmacological or behavior management techniques.
A wide-ranging strategy to identify both published and unpublished studies was a strength of this review. Two authors independently analyzed the studies to be included in this review along with manual hand-searching of the references of the selected articles to limit the risk of selection bias.
Despite the authors’ best efforts, our review is limited by its exclusion of articles in languages other than English. Articles in languages other than English were excluded due to the lack of translational resources and this may have led to publication bias. Moreover, few studies have examined DA in children and adolescents with learning disabilities. Further studies on this population may help to develop an anxiety-measuring tool that could aid in communication and provide effective care. Future studies should adhere to the guidelines of the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) for high-quality reporting. Research aimed at breaking down barriers to adequate dental care should examine dental anxiety trends over time in a population. Finally, the findings of this review must be interpreted with caution owing to the high risk of bias seen in the studies. The reported prevalence may underestimate the real prevalence, as the attrition bias was high for all the included studies. Information regarding the internal validity of the studies was unclear. Most studies did not have details on taking confounding variables into account. Without correcting for potential confounders, the analysis may skew the estimates of the actual effect. The external validity of the study is unclear, reducing the confidence in applying the findings of this review to other populations. The characteristics of the study group were mentioned in most studies. However, reporting on the other criteria for external validity was limited.
Conclusions
Dental anxiety is a universal phenomenon influenced by various cultural features. Based on limited evidence, mild dental anxiety appears common in the Saudi population, especially in the northern region. Women, young adolescents, and university students reported a higher prevalence of dental anxiety. A clinician needs to be aware of a patient’s dental anxiety level and institute anxiety-reducing measures to encourage dental care and compliance. The findings of this systematic review can bridge the gap between anxious patients and clinicians. These results can help guide future researchers in the development and validation of newer anxiety measures to aid in effective communication and delivering quality oral healthcare.
Figures
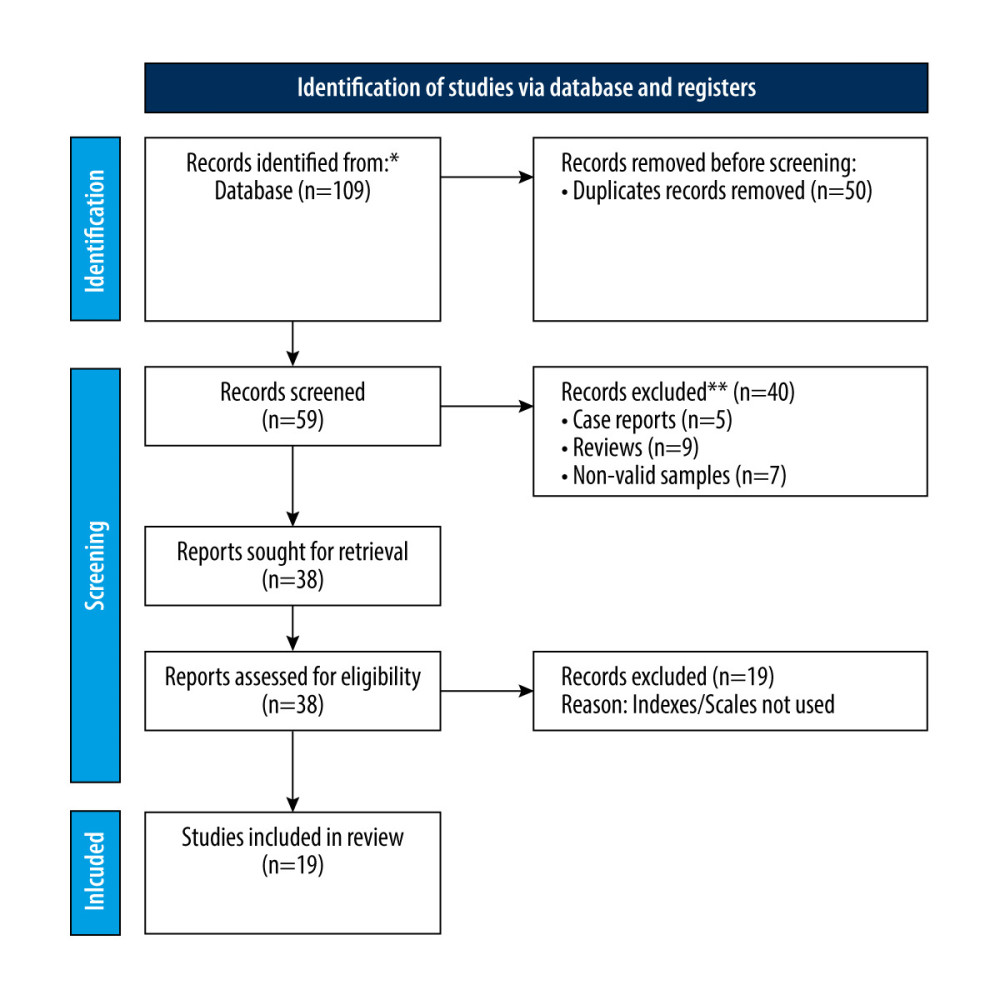 Figure 1. Flow chart depicting the study selection via databases and registries.
Figure 1. Flow chart depicting the study selection via databases and registries. 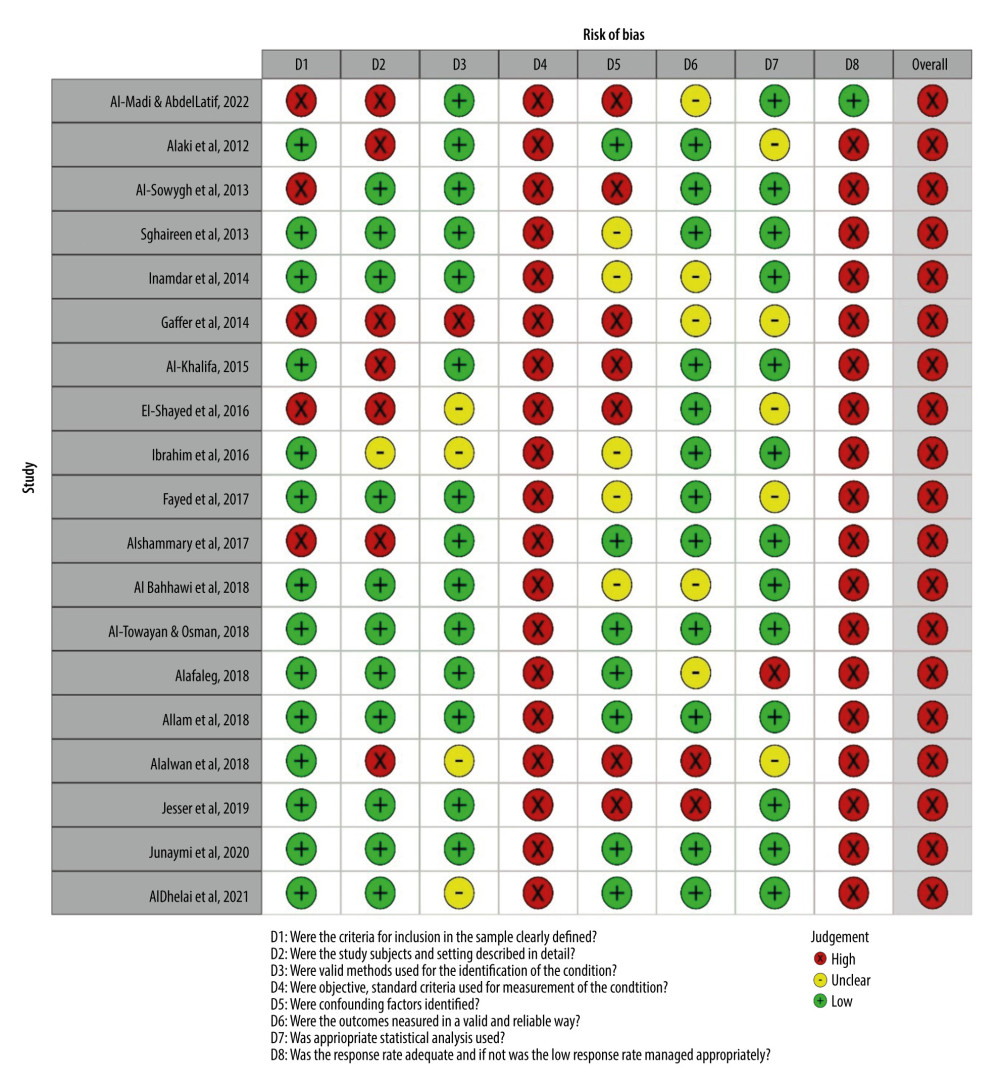 Figure 2. Risk of bias ratings based on Joanna Briggs Institute Critical Appraisal Tools.
Figure 2. Risk of bias ratings based on Joanna Briggs Institute Critical Appraisal Tools. 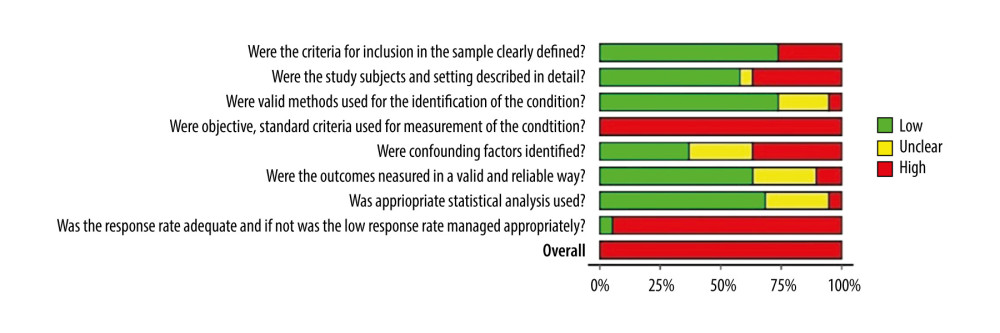 Figure 3. Summary of quality assessment.
Figure 3. Summary of quality assessment. 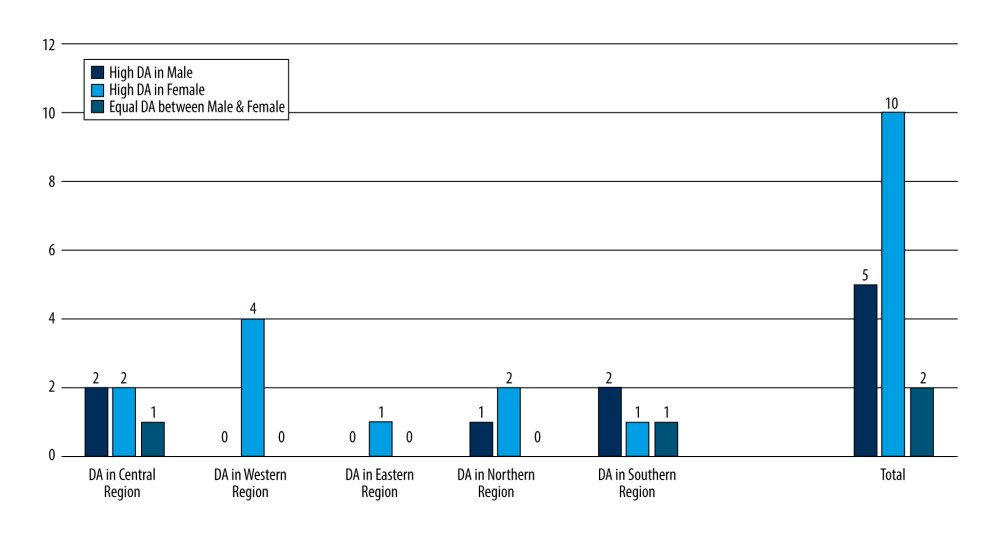 Figure 4. Number of studies that indicated the presence of dental anxiety levels among males and females in all regions of the Kingdom of Saudi Arabia.
Figure 4. Number of studies that indicated the presence of dental anxiety levels among males and females in all regions of the Kingdom of Saudi Arabia. 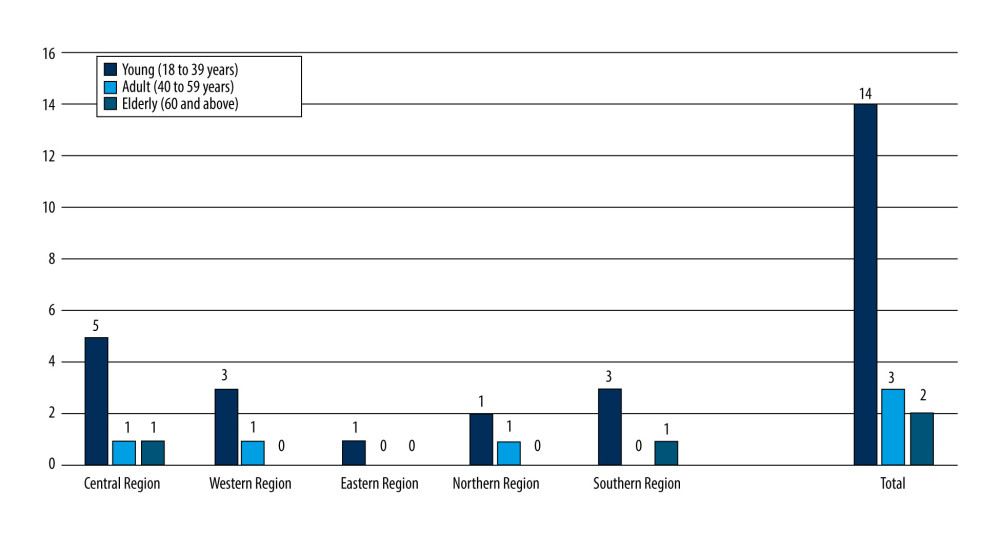 Figure 5. Percentage of dental anxiety among different age groups in all regions of the Kingdom of Saudi Arabia.
Figure 5. Percentage of dental anxiety among different age groups in all regions of the Kingdom of Saudi Arabia. 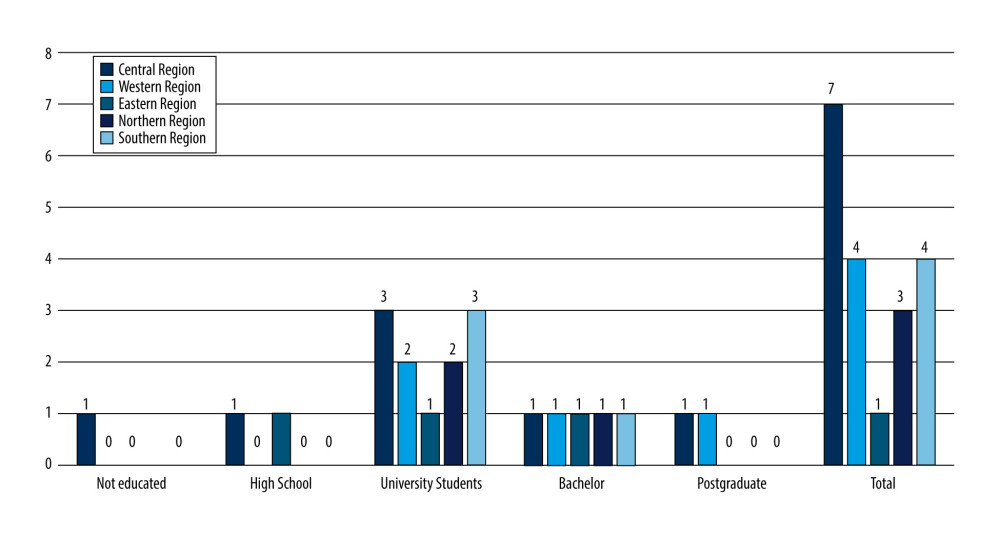 Figure 6. Number of studies that reported high levels of dental anxiety in relation to the level of education among different regions of the Kingdom of Saudi Arabia.
Figure 6. Number of studies that reported high levels of dental anxiety in relation to the level of education among different regions of the Kingdom of Saudi Arabia. 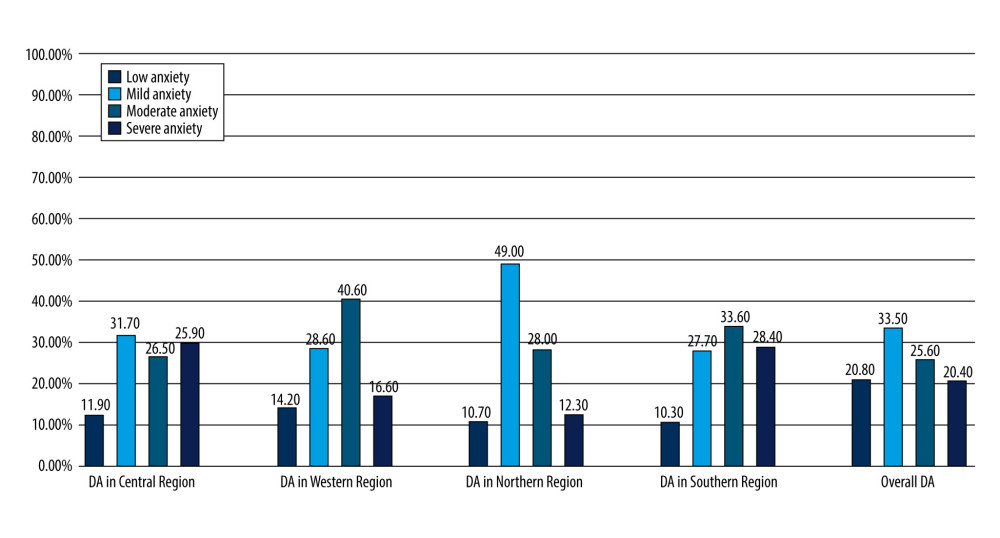 Figure 7. Percentage of dental anxiety levels in all regions of the Kingdom of Saudi Arabia.
Figure 7. Percentage of dental anxiety levels in all regions of the Kingdom of Saudi Arabia. References
1. Valdes-Stauber J, Hummel K, The relationship between dental anxiety and other kinds of anxiety: A naturalistic, cross-sectional and comparative study: BMC Psychol, 2021; 9(1); 184
2. Liddell A, Locker D, Gender and age differences in attitudes to dental pain and dental control: Community Dent Oral Epidemiol, 1997; 25; 314-18
3. Moore R, Birn H, Kirkegaard E, Prevalence and characteristics of dental anxiety in Danish adults: Community Dent Oral Epidemiol, 1993; 21; 292-96
4. Sukumaran I, Taylor S, Thomson WM, The Prevalence and impact of dental anxiety among adult New Zealanders: Int Dent J, 2021; 71; 122-26
5. Grisolia BM, dos Santos APP, Dhyppolito IM, Prevalence of dental anxiety in children and adolescents globally: A systematic review with meta-analyses: Int J Paediatr Dent, 2021; 31; 168-83
6. Hakeberg M, Berggren U, Carlsson SG, Prevalence of dental anxiety in an adult population in a major urban area in Sweden: Community Dent Oral Epidemiol, 1992; 20; 97-101
7. Armfield JM, Stewart JF, Spencer AJ, The vicious cycle of dental fear: Exploring the interplay between oral health, service utilization and dental fear: BMC Oral Health, 2007; 7; 1
8. De Jongh A, Adair P, Meijerink-Anderson M, Clinical management of dental anxiety: What works for whom?: Int Dent J, 2005; 55; 73-80
9. Cohen SM, Fiske J, Newton JT, The impact of dental anxiety on daily living: Br Dent J, 2000; 189; 385-90
10. Eitner S, Wichmann M, Paulsen A, Holst S, Dental anxiety – an epidemiological study on its clinical correlation and effects on oral health: J Oral Rehabil, 2006; 33; 588-93
11. McGrath C, Broder H, Wilson-Genderson M, Assessing the impact of oral health on the life quality of children: Implications for research and practice: Community Dent Oral Epidemiol, 2004; 32; 81-85
12. Liu Y, Huang X, Yan Y, Dental fear and its possible relationship with periodontal status in Chinese adults: A preliminary study: BMC Oral Health, 2015; 15; 18
13. Olak J, Saag M, Honkala S, Children’s dental fear in relation to dental health and parental dental fear: Stomatologija, 2013; 15; 26-31
14. Seligman LD, Hovey JD, Chacon K, Ollendick TH, Dental anxiety: An understudied problem in youth: Clin Psychol Rev, 2017; 55; 25-40
15. Moore R, Brodsgaard I, Dentists’ perceived stress and its relation to perceptions about anxious patients: Community Dent Oral Epidemiol, 2001; 29; 73-78
16. Brahm C-O, Lundgren J, Carlsson SG, Dentists’ views on fearful patients. Problems and promises: Swed Dent J, 2012; 36; 79-89
17. Halonen H, Salo T, Hakko H, Räsänen P, The association between dental anxiety, general clinical anxiety and depression among Finnish university students: Oral Health Dent Manag, 2014; 13; 320-25
18. Locker D, Psychosocial consequences of dental fear and anxiety: Community Dent Oral Epidemiol, 2003; 31; 144-51
19. Crego A, Carrillo-Díaz M, Armfield JM, Romero M, From public mental health to community oral health: The impact of dental anxiety and fear on dental status: Front Public Health, 2014; 2; 16
20. Moore R, Brødsgaard I, Rosenberg N, The contribution of embarrassment to phobic dental anxiety: A qualitative research study: BMC Psychiatry, 2004; 4; 10
21. Berggren U: Dental fear and avoidance: A study of etiology, consequences and treatment, 1984
22. Shim Y-S, Kim A-H, Jeon E-Y, An S-Y, Dental fear & anxiety and dental pain in children and adolescents; A systemic review: J Dent Anesth Pain Med, 2015; 15; 53-61
23. Talo Yildirim T, Dundar S, Bozoglan A, Is there a relation between dental anxiety, fear and general psychological status?: PeerJ, 2017; 5; e2978
24. Humphris GM, Dyer TA, Robinson PG, The modified dental anxiety scale: UK general public population norms in 2008 with further psychometrics and effects of age: BMC Oral Health, 2009; 9; 20
25. do Nascimento DL, da Silva Araújo AC, Gusmão ES, Cimões R, Anxiety and fear of dental treatment among users of public health services: Oral Health Prev Dent, 2011; 9; 329-37
26. Stabholz A, Peretz B, Dental anxiety among patients prior to different dental treatments: Int Dent J, 1999; 49; 90-94
27. Dadalti MT, Cunha AJ, Souza TG, Anxiety about dental treatment – a gender issue: Acta Odontol Latinoam, 2021; 34(2); 195-200
28. Peretz B, Efrat J, Dental anxiety among young adolescent patients in Israel: Int J Paediatr Dent, 2000; 10; 126-32
29. Kamal AT, Sukhia RH, Ghandhi D, Sukhia HR, Stress and anxiety among dental practitioners during the COVID-19 pandemic: A cross-sectional survey: Dent Med Probl, 2021; 58(2); 139-46
30. Nardi GM, Grassi R, Grassi FR, How did the COVID-19 pandemic effect dental patients? An Italian observational survey study: Healthcare, 2021; 9(12); 1748
31. Carrillo-Diaz M, Lacomba-Trejo L, del Valle-González A, Anxiety and facial self-contacts: possible impact on COVID-19 transmission in dental practice: BMC Oral Health, 2021; 21(1); 200
32. Nikolić M, Mitić A, Petrović J, COVID-19: Another cause of dental anxiety?: Med Sci Monit, 2022; 28; e936535
33. Al Moaleem MM, Anxiety during COVID-19 among Saudi Arabian population: A systematic review: World J Dent, 2022; 13(1); 87-94
34. Appukuttan DP, Strategies to manage patients with dental anxiety and dental phobia: Literature review: Clin Cosmet Investig Dent, 2016; 8; 35-50
35. Corah NL, Gale EN, Illig SJ, Assessment of a dental anxiety scale: J Am Dent Assoc, 1978; 97; 816-19
36. Humphris GM, Morrison T, Lindsay SJ, The modified dental anxiety scale: Validation and United Kingdom norms: Community Dent Health, 1995; 12; 143-50
37. Ronis DL, Hansen CH, Antonakos CL, Equivalence of the original and revised dental anxiety scales: J Dent Hyg, 1995; 69(6); 270-72
38. Kleinknecht RA, Thorndike RM, McGlynn FD, Harkavy J, Factor analysis of the dental fear survey with cross-validation: J Am Dent Assoc, 1984; 108; 59-61
39. Lovibond SH, Lovibond PF, Manual for the depression anxiety stress scales: Psychology Foundation of Australia, 1996
40. Lovibond PF, Lovibond SH, The structure of negative emotional states: Comparison of the Depression Anxiety Stress Scales (DASS) with the Beck Depression and Anxiety Inventories: Behav Res Ther, 1995; 33; 335-43
41. Garbee WH, Zucker SB, Selby GR, Perceived sources of stress among dental students: J Am Dent Assoc, 1980; 100; 853-57
42. La Greca AM, Ingles CJ, Lai BS, Marzo JC, Social Anxiety Scale for Adolescents: Factorial invariance across gender and age in Hispanic American adolescents: Assessment, 2015; 22; 224-32
43. Neverlien PO, Assessment of a single-item dental anxiety question: Acta Odontol Scand, 1990; 48; 365-69
44. Goh EZ, Beech N, Johnson NR, Dental anxiety in adult patients treated by dental students: A systematic review: J Dent Educ, 2020; 84; 805-11
45. The Joann Briggs: Joanna Briggs Institute Critical Appraisal Tools for use in Analytical Cross-Sectional Studies, 2017 https://jbi.global/sites/default/files/2019-05/JBI_Critical_Appraisal-Checklist_for_Analytical_Cross_Sectional_Studies2017_0.pdf
46. Hakeem , Bhayat , Shaar A, Qobaly A, Self-assessment of dental anxiety and fear among dental students in a Saudi Arabian college: Br J Med Med Res, 2016; 16; 1-7
47. Ibrahim NK, Al-Jdani M, Al-Aamoudi N, Sukkar S, Anxiety due to dental procedures and treatment among adult patients attending outpatient clinics in King Abdulaziz University Hospital, Jeddah, Saudi Arabia: J Med Res, 2016; 2; 35-40
48. Alaki S, Alotaibi A, Almabadi E, Alanquri E, Dental anxiety in middle school children and their caregivers: Prevalence and severity: J Dent Oral Hyg, 2012; 4; 6-11
49. Al-Khalifa KS, Prevalence of dental anxiety in two major cities in the Kingdom of Saudi Arabia: Saudi J Med Med Sci, 2015; 3; 135
50. Gaffar BO, Alagl AS, Al-Ansari AA, The prevalence, causes, and relativity of dental anxiety in adult patients to irregular dental visits: Saudi Med J, 2014; 35; 598-603
51. Fayad MI, Elbieh A, Baig MN, Alruwaili SA, Prevalence of dental anxiety among dental patients in Saudi Arabia: J Int Soc Prev Community Dent, 2017; 7; 100-4
52. Sghaireen MG, Zwiri AMA, Alzoubi IA, Anxiety due to dental treatment and procedures among university students and its correlation with their gender and field of study: Int J Dent, 2013; 2013; 1-5
53. Alalwan SAM, Albader FNB, Alkhalaf ZAH, Dental anxiety among patients undergoing different dental treatments in college of dentistry, Riyadh Elm University: Saudi J Oral Dent Res, 2018; 3; 379-85
54. Allam R, Allam Y, Al-Samhan AZ, Al-Ghazi M, Gender differences in anxiety levels about dentistry in Saudi dental college students: EC Dent Sci, 2018; 17; 663-67
55. Al-Towayan A, Osman KH, Prevalence of dental anxiety among medical and dental undergraduates in Gassim University: Inte J Medi Heal Res, 2018; 4; 15-18
56. Inamdar A, Alwadaani M, Asiri A, Dental anxiety in medical and dental undergraduates at Jazan University: J Oral Heal Res, 2014; 4; 25
57. AlDhelai TA, Al-Ahmari MM, Adawi HA, Dental anxiety and fear among patients in Jazan, Kingdom of Saudi Arabia: A cross-sectional study: J Contemp Dent Pract, 2021; 22; 549-56
58. AL Jasser R, Almashaan G, Alwaalan H, Dental anxiety among dental, medical, and nursing students of two major universities in the central region of the Kingdom of Saudi Arabia: A cross-sectional study: BMC Oral Health, 2019; 19; 56
59. Al-Sowygh ZH, Alfadley AA, Al-Saif MI, Al-Wadei SH, Perceived causes of stress among Saudi dental students: King Saud Univ J Dent Sci, 2013; 4; 7-15
60. Al-Madi EM, AbdelLatif H, Assessment of dental fear and anxiety among adolescent females in Riyadh, Saudi Arabia: Saudi Dent J, 2002; 14; 77-81
61. Alafaleg R, Buraidah Q, Arabia S, Prevalence of dental anxiety among Saudi population in Buraiydah: Dent Students’ Res, 2011; 24-32
62. Alshammary M, Alhumaid M, Alnejeem G, Osman M, Dental anxiety among medical field students in University of Hail, Saudi Arabia: Sch J Dent Sci, 2017
63. Jumaymi AK, Faqehi WH, Hamdi SA, Level of dental anxiety and its relation to Khat Chewing in Jazan population: A cross-sectional study: J Contemp Dent Pract, 2020; 21; 253-60
64. AlBahhawi T, Albasheer OB, Makeen AM, Depression, anxiety, and stress and their association with khat use: A cross-sectional study among Jazan University students, Saudi Arabia: Neuropsychiatr Dis Treat, 2018; 14; 2755-61
65. White AM, Giblin L, Boyd LD, The prevalence of dental anxiety in dental practice settings: Am Dent Hyg Assoc, 2017; 91; 30-34
66. Madfa AA, Amran AG, Al-Sanabani FA, prevalence of dental anxiety and fear among medical students at University of Thamar: Am J Heal Res, 2015; 3; 5-9
67. Suhani RD, Suhani MF, Badea ME, Dental anxiety and fear among a young population with hearing impairment: Clujul Med, 2016; 89; 143-49
68. Kakkar M, Wahi A, Thakkar R, Prevalence of dental anxiety in 10–14 years old children and its implications: J Dent Anesth Pain Med, 2016; 16; 199
69. Caltabiano ML, Croker F, Page L, Dental anxiety in patients attending a student dental clinic: BMC Oral Health, 2018; 18; 48
70. Saatchi M, Abtahi M, Mohammadi G, The prevalence of dental anxiety and fear in patients referred to Isfahan Dental School, Iran: Dent Res J (Isfahan), 2015; 12; 248-53
71. Ihara Y, Fukuda K-I, Saita N, Ichinohe T, Male gender and high trait anxiety are two major factors associated with severe dental fear and avoidance: Anesth Prog, 2018; 65; 177-80
72. Folayan MO, Idehen EE, Ojo OO, The modulating effect of culture on the expression of dental anxiety in children: A literature review: Int J Paediatr Dent, 2004; 14; 241-45
73. Glazman J, Dental anxiety: Personal and media influences on the perception of dentistry: Thesis, 2014, Honors College, Pace University
74. Humphris G, King K, The prevalence of dental anxiety across previous distressing experiences: J Anxiety Disord, 2011; 25; 232-36
75. Gujjar KR, Van Wijk A, Kumar R, De Jongh A, Are technology-based interventions effective in reducing dental anxiety in children and adults? A systematic review: J Evid Based Dent Pract, 2019; 19; 140-55
Figures
 Figure 1. Flow chart depicting the study selection via databases and registries.
Figure 1. Flow chart depicting the study selection via databases and registries. Figure 2. Risk of bias ratings based on Joanna Briggs Institute Critical Appraisal Tools.
Figure 2. Risk of bias ratings based on Joanna Briggs Institute Critical Appraisal Tools. Figure 3. Summary of quality assessment.
Figure 3. Summary of quality assessment. Figure 4. Number of studies that indicated the presence of dental anxiety levels among males and females in all regions of the Kingdom of Saudi Arabia.
Figure 4. Number of studies that indicated the presence of dental anxiety levels among males and females in all regions of the Kingdom of Saudi Arabia. Figure 5. Percentage of dental anxiety among different age groups in all regions of the Kingdom of Saudi Arabia.
Figure 5. Percentage of dental anxiety among different age groups in all regions of the Kingdom of Saudi Arabia. Figure 6. Number of studies that reported high levels of dental anxiety in relation to the level of education among different regions of the Kingdom of Saudi Arabia.
Figure 6. Number of studies that reported high levels of dental anxiety in relation to the level of education among different regions of the Kingdom of Saudi Arabia. Figure 7. Percentage of dental anxiety levels in all regions of the Kingdom of Saudi Arabia.
Figure 7. Percentage of dental anxiety levels in all regions of the Kingdom of Saudi Arabia. In Press
15 Apr 2024 : Laboratory Research
The Role of Copper-Induced M2 Macrophage Polarization in Protecting Cartilage Matrix in OsteoarthritisMed Sci Monit In Press; DOI: 10.12659/MSM.943738
07 Mar 2024 : Clinical Research
Knowledge of and Attitudes Toward Clinical Trials: A Questionnaire-Based Study of 179 Male Third- and Fourt...Med Sci Monit In Press; DOI: 10.12659/MSM.943468
08 Mar 2024 : Animal Research
Modification of Experimental Model of Necrotizing Enterocolitis (NEC) in Rat Pups by Single Exposure to Hyp...Med Sci Monit In Press; DOI: 10.12659/MSM.943443
18 Apr 2024 : Clinical Research
Comparative Analysis of Open and Closed Sphincterotomy for the Treatment of Chronic Anal Fissure: Safety an...Med Sci Monit In Press; DOI: 10.12659/MSM.944127
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952