13 September 2022: Clinical Research
A Case-Control Study of the Effects of Implementing the Registered Nurses’ Association of Ontario Guidelines for the Assessment and Management of Postoperative Pain and the Use of Relaxation Therapy in 312 Patients with Bone and Soft-Tissue Malignancy
Qian Gao12ABCDEF, Qi Xu12BC, Xiaowei Zhou12D, Zhaonong Yao12F, Yuhong Yao12AEFG*DOI: 10.12659/MSM.937496
Med Sci Monit 2022; 28:e937496
Abstract
BACKGROUND: The present study aimed to investigate the effects of implementing the Registered Nurses’ Association of Ontario (RNAO) guidelines for the management of postoperative pain and the use of Jacobson’s relaxation technique (JRT) in patients with bone and soft-tissue malignancy at a single center in China.
MATERIAL AND METHODS: A total of 312 patients were recruited and randomly divided into 2 groups. In the intervention group, the RNAO pain-management technique of JRT was adopted, while the control group received the standard institutional nursing management. Pain scores after the operation, according to the Numerical Rating Scale (NRS) combined with the Wong-Baker Faces Pain Rating Scale and Short-Form McGill Pain Questionnaire, were compared between the 2 groups. Nursing satisfaction was compared as well.
RESULTS: At 6, 24, and 72 h after the operation, the NRS scores combined with the Wong-Baker Faces Pain Rating Scale in the intervention group were significantly lower than those in the control group (P<0.001); 72 h after the operation, the Pain Rating Index, Visual Analogue Scale, present pain intensity, and total scores for the intervention group were significantly lower than those for the control group (P<0.001 for all 4 scores). The scores reported from the patients for nursing response and consequent care (P<0.001), nursing competence (P=0.029), and surgical pain-control satisfaction (P<0.001) in the intervention group were also significantly higher than those in the control group.
CONCLUSIONS: JRT can improve postoperative pain-control and nursing satisfaction in patients with malignant bone and soft-tissue tumors. These data suggest a benefit for application of JRT in clinical care.
Keywords: Bone Neoplasms, pain management, Sarcoma, Case-Control Studies, Humans, Nurses, Ontario, Pain, Postoperative, Relaxation Therapy
Background
Pain, an unpleasant sensory and emotional experience caused by actual or potential tissue damage, has become the fifth most important vital sign. In the clinical care of patients with bone and soft-tissue malignancy, postoperative pain control is one of the important indicators used to evaluate the quality of nursing care. However, pain control for patients in China is still less than satisfactory, warranting a more standardized and effective pain care management strategy [1,2]. The third edition of the Registered Nurses’ Association of Ontario (RNAO) Best Practice Guideline on the Assessment and Management of Pain (RNAO pain guideline), published in 2013, is designed to apply to all domains of nursing practice, including clinical, administration, and education, to assist nurses in becoming more comfortable, confident, and competent when assessing and managing people with the presence, or risk of, any type of pain. Up to now, there has been no detailed national guideline for pain management for clinical nursing in China. Instead, separate institutional practice guidelines have been used. RNAO pain guidelines have achieved a decrease in the prevalence and intensity of pain in the clinical setting [3,4]. Therefore, it is necessary to explore multimodal analgesia following the RNAO pain guidelines for postoperative pain management in patients with bone and soft-tissue malignancy. In the RNAO guidelines, non-pharmacological regimens are emphasized along with pharmacological approaches. One such technique, non-invasive Jacobson’s relaxation technique (JRT), warrants evaluation in the multimodal analgesia routine.
JRT was originally proposed by Dr. Edmund Jacobson, an American physician, and was originally used to help reduce stress, anxiety, and depression [5]. JRT is a type of physical therapy that includes the sequential tightening and relaxing of specific muscle groups. In further clinical exploration, previous studies have indicated that JRT can help patients with postoperative anxiety relief and pain control [6–8]. JRT emphasizes whole-body progressive muscle relaxation, implying a potentially positive effect on pain control in patients with bone and soft-tissue malignancy, especially those with low pain scores.
The present case-control study aimed to investigate the effects of implementing the RNAO guidelines for the assessment and management of postoperative pain and the use of relaxation therapy in 312 patients with bone and soft-tissue malignancy at a single center in China between January and August, 2021.
Material and Methods
ETHICS APPROVAL:
This study was approved by the Ethics Board (IRB) of the Second Affiliated Hospital of Zhejiang University School of Medicine (SAHZU). The original and translated ethics approval documentation was provided to the editor of the journal. This study was conducted in accordance with the principles of the Helsinki Declaration. All of the patients or the guardians of children signed the informed consent before they participated in the study. The participants were fully aware of the procedure of the study.
PATIENTS:
The study encompassed 312 patients with bone and soft-tissue malignancy undergoing surgery at SAHZU Bone Tumor Center, Department of Orthopaedics from January 2021 to August 2021. The patients were randomly divided into an intervention group and control group with 156 cases in each group. The study participants joined this study according to the following inclusion criteria: clear indications for surgery resulting in surgical treatment, ability to understand and communicate, and reception of patient-controlled analgesia after surgery. However, those who had mental illness or cognitive impairment, experienced severe postoperative complications, dropped out of followup, or could not complete the JRT were excluded from the study.
PAIN EVALUATION METHODS:
Numerical Rating Scale (NRS): patients are asked to circle the number between 0 and 10 that fits best to their pain intensity. Zero usually represents “no pain at all” whereas the upper limit represents “the worst pain ever possible”; 1–3 represents mild pain, 4–6 represents moderate pain, and 7–10 represents severe pain.
Wong-Baker Faces Pain Rating Scale: this scale illustrates face cartoons ranging from a happy face at 0 score, representing “no pain at all”, to a crying face at 10 score, which indicates “the worst pain one can imagine”. According to the face cartoons and written descriptions, the patient chooses the face cartoon that best fits their pain intensity. This method was applied only for patients unable to accomplish the NRS system.
Short-Form McGill Pain Questionnaire (SF-MPQ): The measure is calculated by summing the point values for responses to 15 questions. Questions 1–11 deal with the sensory dimension of pain (Pain Rating Index, PRI). Questions 12–15 deal with the affective dimension of pain. Subscores for the sensory and affective dimensions are calculated, in addition to a total McGill Pain Score. In addition, there is a Visual Analogue Scale (VAS) for pain intensity and a final question about present pain intensity (PPI). Higher scores generally correspond to a worse subjective experience of pain.
INTERVENTIONS:
Control group: The control group adopted a routine nursing management method described by an institutional guideline in SAHZU. Routine pain assessment and treatment were carried out for postoperative patients according to the “Pain Assessment and Management System” of the authors’ hospital. For patients with a pain score of 1–3, nurses gave psychological support. For patients with a pain score ≥4, timely assessment, instant report to the physician, and pain relief therapeutics would be done according to the physician’s advice. Patients with a pain score ≥7 should be treated as an emergency. Reassessment was required after the pain medicines were taken.
Intervention group: The intervention group adopted the RNAO pain-management protocol of JRT. A multidisciplinary pain-management team was established, including orthopedists, anesthesiologists, and pain-control specialist nurses. Orthopedists are responsible for formulating primary analgesia strategies to alleviate pain based on the results of pain assessment and contacting anesthesiologists for assistance when necessary. Anesthesiologists have key roles in dealing with ineffective postoperative pain control. Pain-control specialist nurses are responsible for the nursing management of pain in patients guided by RNAO pain guidelines, including assessment, planning, implementation, and evaluation. The care plan needs to be comprehensive, and based on the patient’s beliefs, knowledge, and understanding. Pain assessment using multi-dimensional assessment tools: NRS, Wong-Baker Faces Pain Rating Scale for patients with difficulty in expressing their pain using the NRS, and the Short-From McGill Pain Questionnaire. Before surgery, pain-control specialist nurses strengthened pain education and psychological intervention by introducing the causes, influences, and prognosis of the pain, as well as the common postoperative analgesia methods. Misconceptions were also addressed, to ease the concerns of patients and their families about postoperative pain. Multimodal analgesia: in addition to patient-controlled analgesia after surgery, non-pharmacological measures should be taken for patients with NRS scores of 1–3. The nurses should also instruct patients to use JRT combined with psychological support. For patients with NRS score ≥4, the multidisciplinary pain-management team formulated a targeted analgesia plan, with a combination of analgesic drugs and regular re-evaluation of the effectiveness of the pain management.
JRT PROCEDURE:
For JRT, the patient starts from the foot muscle group and moves to the shoulder, continuously contracting and relaxing 16 muscle groups in the body twice a day for 10 min each time. Each muscle group is contracted for 10 s, followed by relaxing the muscle group for 20 s, and consequently moving on to the contraction-relaxation cycle of the next muscle group. Muscle groups that are affected by the surgery or cannot complete this relaxation are skipped, with the patient moving on to the next muscle group.
OUTCOME MEASUREMENT:
The effectiveness of pain control of the 2 groups was compared. The NRS combined with the Wong-Baker Faces Pain Rating Scale was used to evaluate the pain intensity on the day of admission and at 6 h, 24 h, and 72 h after the operation. The SF-MPQ was used to evaluate the pain intensity on the day of admission and 72 h after the operation. Satisfaction with the nursing was evaluated using a self-made questionnaire filled out by members of the 2 groups of patients when discharged. The content of the self-made questionnaire included 6 parts: basic information, overall satisfaction with the nursing, satisfaction with nurse-patient communication, satisfaction with nursing response and care, satisfaction with nursing competence, and satisfaction with surgical pain control. The degree of satisfaction was divided into 5 levels: poor (1 point), fair (2 points), good (3 points), very good (4 points), and excellent (5 points).
STATISTICAL METHODS:
In this study, Epidata3.1 was used for data input, and SPSS21.0 was used for data analysis. The t-test was used to compare the NRS score, Wong-Baker Faces Pain Rating Scale score, and SF-MPQ score between the intervention group and the control group, as used in Tables 1–3. The t-test was used to compare the satisfaction with nursing care in the 2 groups, as shown in Table 4. P<0.05 was considered statistically significant.
Results
BASELINE CHARACTERISTICS:
Clinical characteristics of the participants at baseline are shown in Table 1. This study included 312 patients, including 169 male and 143 female patients; the ages ranged from 12 to 75 years old, with an average age of 46.43±20.26 years; among the 312 patients, 213 had primary bone and soft-tissue malignancy, and 99 had metastatic bone and soft-tissue malignancy. The mean age of the intervention group was 46.69±20.58, while the mean age of the control group was 46.17±20.00. There was no statistically significant difference between the 2 groups of patients in terms of sex, age, or tumor type distribution (P>0.05).
PAIN SCORES:
As is shown in Table 2, the results of the study showed that there was no statistically significant difference between the 2 groups in NRS scores combined with the Wong-Baker Faces Pain Rating Scale scores on the day of admission. The scores in the intervention group and control group were 5.50±2.13 and 5.63±1.90, respectively (P=0.287). However, 6 h, 24 h, and 72 h after the operation, the NRS combined with the Wong-Baker Faces Pain Rating Scale scores in the intervention group were significantly lower than those in the control group (P<0.001). At the timepoint of 72 h after operation, the scores were 2.76±1.12 in the intervention group, while they were 3.47±1.47 in the control group.
In addition, the PRI, VAS, PPI, and total scores of the SF-MPQ on the day of admission were not statistically different between the intervention group and the control group, with P values of 0.144, 0.287, 0.152, and 0.470, respectively. However, 72 h after the operation, the PRI, VAS, PPI, and total scores of the SF-MPQ were significantly lower than those of the control group (P<0.001 for all of the 4 scores above; Table 3). The SF-MPQ scores in the intervention group 72 h after operation were 5.54±2.86, 2.77±1.13, 1.55±0.98, and 9.87±3.22, whereas they were 7.43±3.56, 3.52±1.45, 2.85±1.17, and 13.78±4.49 in the control group (P<0.001).
NURSING SATISFACTION:
The study showed that the patients in the 2 groups were satisfied with the following parameters: “the general nursing during hospitalization”, “the nurses take the initiative to inform regarding relevant matters”, “the nurses respond and help in a timely manner when they encounter problems”, “nurses’ working competence”, and “postoperative pain management and control”, with average scores between “very good” and “excellent”. There was no statistically significant difference between the 2 groups in terms of general nursing (P=0.367) and the level to which the patients felt they were adequately informed about the nursing process (nurse-patient communication) (P=0.112), but the intervention group showed a significantly higher score in nursing response and care (P<0.001), nursing competence (P=0.029), and surgical pain control (P<0.001) (Table 4).
Discussion
LIMITATIONS:
This study had potential limitations. An important limitation of this project was that the effect estimates in this model are based on 312 patients. This sample size is small, and also, the study was performed at only one center. Therefore, a larger sample size and a multiple-center double-blinded controlled trial is needed for future studies. Secondly, we only investigated the short-term results of this model, and we could not draw any conclusions about longer-term effects, which deserve future research through randomized clinical trials.
Conclusions
The RNAO pain guidelines method JRT can improve postoperative pain-control and nursing satisfaction in patients with malignant bone and soft-tissue tumors. It is therefore suggested that this method be widely promoted and applied in clinical nursing. Furthermore, choosing appropriate tools to assess and manage postoperative pain according to the types of diseases and the characteristics of the patients can help patients reduce pain more efficiently.
Tables
Table 1. Patient characteristics. There was no statistical difference between the 2 groups regarding sex, age, or tumor types.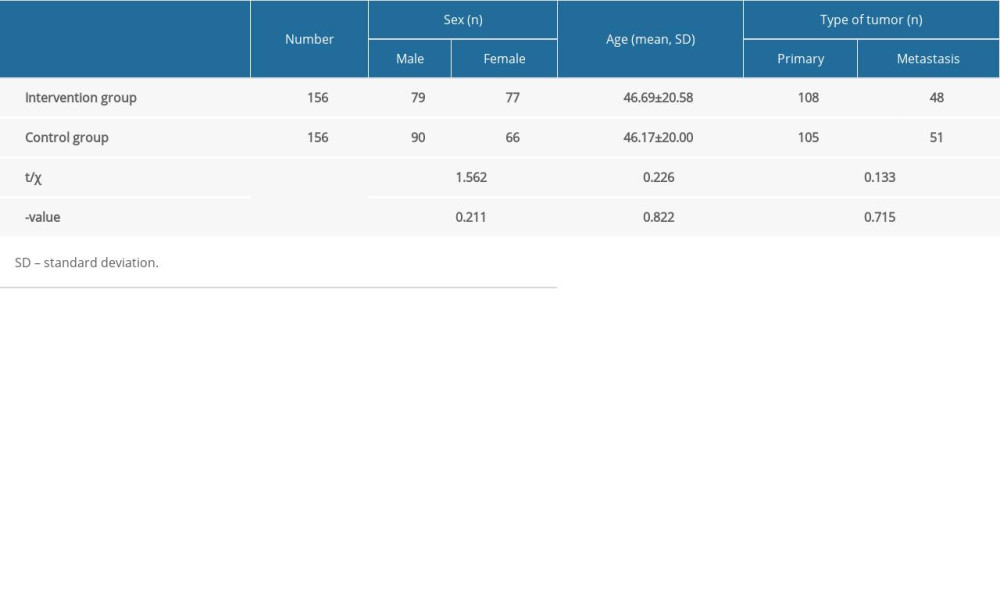 Table 2. Pain scores (NRS system in combination with Wong-Baker rating scale). Patients in the intervention group had significantly lower scores when compared with individuals in the control group.
Table 2. Pain scores (NRS system in combination with Wong-Baker rating scale). Patients in the intervention group had significantly lower scores when compared with individuals in the control group.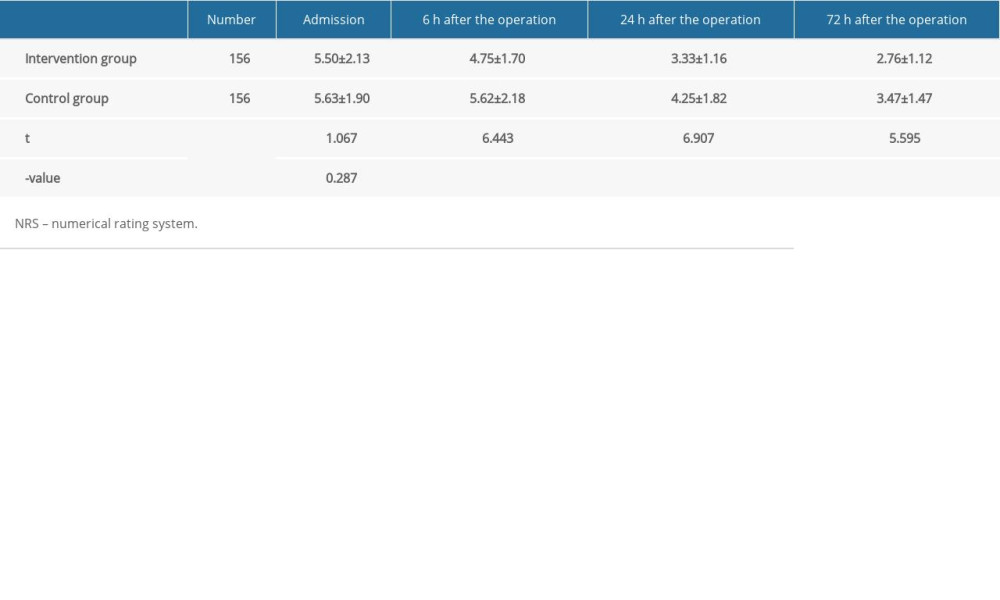 Table 3. The SF-MPQ scale was used to compare the scores between the intervention group and control group. The scores in the SF-MPQ scale were significantly lower in the intervention group.
Table 3. The SF-MPQ scale was used to compare the scores between the intervention group and control group. The scores in the SF-MPQ scale were significantly lower in the intervention group.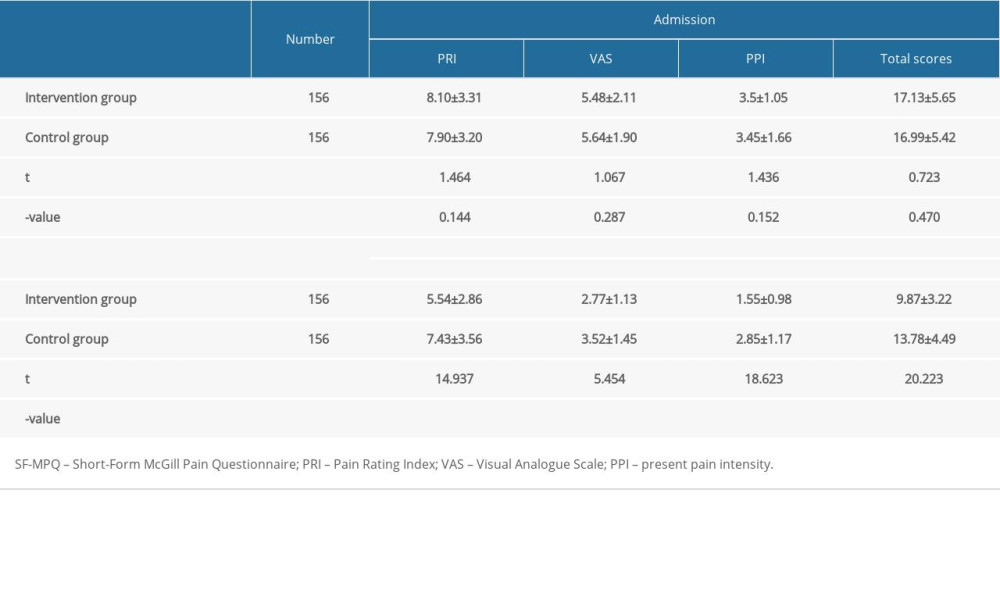 Table 4. The nursing satisfaction status was compared between the 2 group. The patients in the intervention group had favorable nursing satisfaction in the aspects of nurse-patient communication, nursing responsiveness and care, nursing competence, and pain control.
Table 4. The nursing satisfaction status was compared between the 2 group. The patients in the intervention group had favorable nursing satisfaction in the aspects of nurse-patient communication, nursing responsiveness and care, nursing competence, and pain control.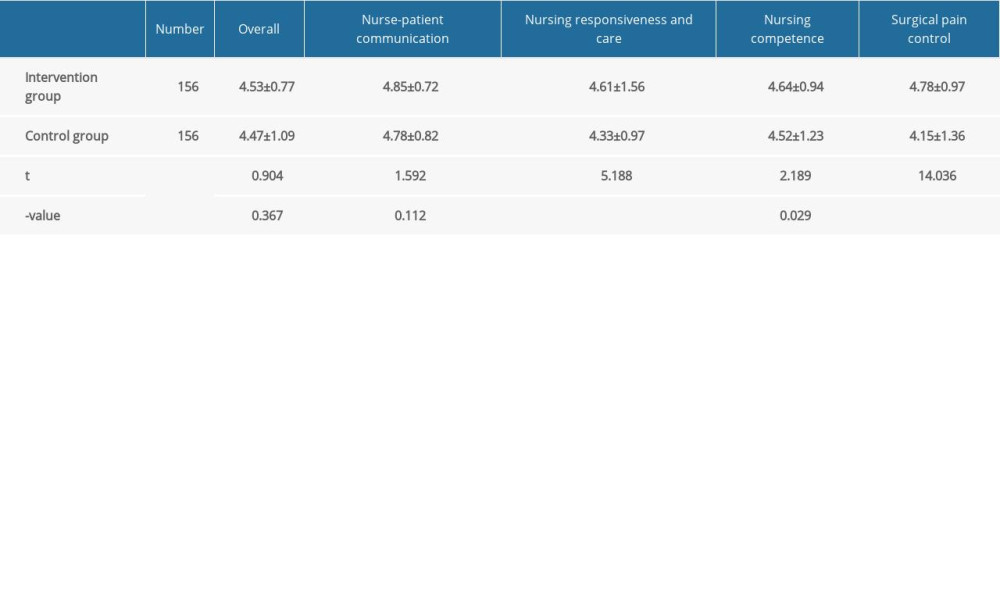
References
1. Soffin EM, YaDeau JT, Enhanced recovery after surgery for primary hip and knee arthroplasty: A review of the evidence: Br J Anaesth, 2016; 117(Suppl 3); iii62-iii72
2. Luo ZY, Yu QP, Zeng WN, Adductor canal block combined with local infiltration analgesia with morphine and betamethasone show superior analgesic effect than local infiltration analgesia alone for total knee arthroplasty: A prospective randomized controlled trial: BMC Musculoskelet Disord, 2022; 23(1); 468
3. Saiz Vinuesa MD, Albornos-Munoz L, Fernandez Nunez ML, Implementation results of the assessment and management of pain guideline within Best Practice Spotlight Organisations (BPSO(R)): Enferm Clin (Engl Ed), 2020; 30(3); 212-21
4. Rolin-Gilman C, Fournier B, Cleverley K, Implementing best practice guidelines in pain assessment and management on a Women’s Psychiatric Inpatient Unit: Exploring patients’ perceptions: Pain Manag Nurs, 2017; 18(3); 170-78
5. Jacobson E, Progressive relaxation: Am J Psychol, 1987; 100(3/4); 522-37
6. Mehnert A, Koch U, Schulz H, Prevalence of mental disorders, psychosocial distress and need for psychosocial support in cancer patients – study protocol of an epidemiological multi-center study: BMC Psychiatry, 2012; 12; 70
7. Paras-Bravo P, Salvadores-Fuentes P, Alonso-Blanco C, The impact of muscle relaxation techniques on the quality of life of cancer patients, as measured by the FACT-G questionnaire: PLoS One, 2017; 12(10); e0184147
8. Paras-Bravo P, Alonso-Blanco C, Paz-Zulueta M, Does Jacobson’s relaxation technique reduce consumption of psychotropic and analgesic drugs in cancer patients? A multicenter pre-post intervention study: BMC Complement Altern Med, 2018; 18(1); 139
9. Kulkarni M, Mallesh M, Wakankar H, Effect of methylprednisolone in periarticular infiltration for primary total knee arthroplasty on pain and rehabilitation: J Arthroplasty, 2019; 34(8); 1646-49
10. Liu H, Gao X, Hou Y, Effects of mindfulness-based stress reduction combined with music therapy on pain, anxiety, and sleep quality in patients with osteosarcoma: Braz J Psychiatry, 2019; 41(6); 540-45
11. Yin M, Li J, Wang J, Observation of the effect of focused psychological intervention combined with standardized pain nursing on postoperative pain levels and depression and anxiety in patients with intestinal obstruction: Dis Markers, 2022; 2022; 2467887
12. Meng X, Yu Y, Effect of rehabilitation nursing under the guidance of the health action process approach model on perioperative nursing effect of artificial hip arthroplasty: Effect on promoting quality of life and postoperative rehabilitation: Comput Math Methods Med, 2022; 2022; 1247002
13. Ramos O, Mierke A, Filler R, Outpatient opioid prescribing habits in pediatric patients with bone sarcomas after undergoing primary tumor resection: J Pediatr Orthop, 2022; 42(5); e501-e6
14. Komatsu S, Okamoto M, Shiba S, Prospective evaluation of quality of life and functional outcomes after carbon ion radiotherapy for inoperable bone and soft tissue sarcomas: Cancers (Basel), 2021; 13(11); 2591
15. Weiss MC, Systemic treatment of soft tissue sarcomas in the geriatric population: Curr Treat Options Oncol, 2022; 23(6); 855-63
16. den Hollander D, Lidington E, Singer S, ‘I thought I had fibroids, and now I don’t’: A mixed method study on health-related quality of life in uterine sarcoma patients: Health Qual Life Outcomes, 2022; 20(1); 65
17. Ruano A, Garcia-Torres F, Galvez-Lara M, Moriana JA, Psychological and non-pharmacologic treatments for pain in cancer patients: A systematic review and meta-analysis: J Pain Symptom Manage, 2022; 63(5); e505-e20
18. Kazak A, Ozkaraman A, The effect of progressive muscle relaxation exercises on pain on patients with sickle cell disease: Randomized controlled study: Pain Manag Nurs, 2021; 22(2); 177-83
19. Dikmen HA, Terzioglu F, Effects of reflexology and progressive muscle relaxation on pain, fatigue, and quality of life during chemotherapy in gynecologic cancer patients: Pain Manag Nurs, 2019; 20(1); 47-53
20. Ozdemir C, Karazeybek E, Soyuncu Y, Relationship between quality of care and patient care outcomes for postoperative pain in major orthopedic surgery: Analytical and cross-sectional study: Clin Nurs Res, 2022; 31(3); 530-40
21. Giordano NA, Seilern Und Aspang J, Baker J, Integration of life care specialists into orthopaedic trauma care to improve postoperative outcomes: A pilot study, 2022 [Online ahead of print]
22. Whale K, Wylde V, Beswick A, Effectiveness and reporting standards of psychological interventions for improving short-term and long-term pain outcomes after total knee replacement: A systematic review: BMJ Open, 2019; 9(12); e029742
23. Patton L, Avsar P, Nugent DL, What is the impact of specialist palliative care outpatient consultations on pain in adult patients with cancer? A systematic review: Eur J Oncol Nurs, 2021; 55; 102034
24. Huang TT, Sung CC, Wang WS, Wang BH, The effects of the empowerment education program in older adults with total hip replacement surgery: J Adv Nurs, 2017; 73(8); 1848-61
25. Zoega S, Ward S, Gunnarsdottir S, Evaluating the quality of pain management in a hospital setting: Testing the psychometric properties of the Icelandic version of the revised American Pain Society patient outcome questionnaire: Pain Manag Nurs, 2014; 15(1); 143-55
26. Sinmaz T, Akansel N, Experience of pain and satisfaction with pain management in patients after a lumbar disc herniation surgery: J Perianesth Nurs, 2021; 36(6); 647-55
27. Subramanian B, Shastri N, Aziz L, ASSIST – Patient satisfaction survey in postoperative pain management from Indian subcontinent: J Anaesthesiol Clin Pharmacol, 2017; 33(1); 40-47
28. Eti Aslan F, Kula Sahin S, Secginli S, Bulbuloglu SPatient satisfaction with nursing practices about postoperative pain management: A systematic review: Agri, 2018; 30(3); 105-15 [in Turkish]
29. Lee CH, Liu JT, Lin SC, Effects of educational intervention on state anxiety and pain in people undergoing spinal surgery: A randomized controlled trial: Pain Manag Nurs, 2018; 19(2); 163-71
30. Chen LY, Sun YC, Cheng CREvaluation of the nurses’ utilization of the pain management information system based on the information system success model: Hu Li Za Zhi, 2022; 69(1); 63-72 [in Chinese]
Tables
 Table 1. Patient characteristics. There was no statistical difference between the 2 groups regarding sex, age, or tumor types.
Table 1. Patient characteristics. There was no statistical difference between the 2 groups regarding sex, age, or tumor types. Table 2. Pain scores (NRS system in combination with Wong-Baker rating scale). Patients in the intervention group had significantly lower scores when compared with individuals in the control group.
Table 2. Pain scores (NRS system in combination with Wong-Baker rating scale). Patients in the intervention group had significantly lower scores when compared with individuals in the control group. Table 3. The SF-MPQ scale was used to compare the scores between the intervention group and control group. The scores in the SF-MPQ scale were significantly lower in the intervention group.
Table 3. The SF-MPQ scale was used to compare the scores between the intervention group and control group. The scores in the SF-MPQ scale were significantly lower in the intervention group. Table 4. The nursing satisfaction status was compared between the 2 group. The patients in the intervention group had favorable nursing satisfaction in the aspects of nurse-patient communication, nursing responsiveness and care, nursing competence, and pain control.
Table 4. The nursing satisfaction status was compared between the 2 group. The patients in the intervention group had favorable nursing satisfaction in the aspects of nurse-patient communication, nursing responsiveness and care, nursing competence, and pain control. In Press
06 Mar 2024 : Clinical Research
Comparison of Outcomes between Single-Level and Double-Level Corpectomy in Thoracolumbar Reconstruction: A ...Med Sci Monit In Press; DOI: 10.12659/MSM.943797
21 Mar 2024 : Meta-Analysis
Economic Evaluation of COVID-19 Screening Tests and Surveillance Strategies in Low-Income, Middle-Income, a...Med Sci Monit In Press; DOI: 10.12659/MSM.943863
10 Apr 2024 : Clinical Research
Predicting Acute Cardiovascular Complications in COVID-19: Insights from a Specialized Cardiac Referral Dep...Med Sci Monit In Press; DOI: 10.12659/MSM.942612
06 Mar 2024 : Clinical Research
Enhanced Surgical Outcomes of Popliteal Cyst Excision: A Retrospective Study Comparing Arthroscopic Debride...Med Sci Monit In Press; DOI: 10.12659/MSM.941102
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








